WellCare of North Carolina is now Carolina Complete Health. Learn more about the merger.
About the Merger Between Carolina Complete Health and
WellCare of North Carolina
As a valued provider in the Carolina Complete Health and WellCare of North Carolina networks, your partnership is essential to our shared mission to transform the health of the communities we serve, one person at a time.
We are excited to share that Carolina Complete Health and WellCare officially combined into a single, statewide health plan on April 1, 2026. The new entity is named Carolina Complete Health and will maintain its Provider-Led Entity governance structure. This transition reinforces our commitment to simplify and strengthen our partnership with you.

To support your success during the transition, we will update this page on a regular basis with important resources, tools, and guidance tailored to providers.
Thank you for your continued dedication to our members and the future of health care in North Carolina.
A Commitment to Provider-Led Managed Care
The statewide PLE will continue to be governed by North Carolina physicians. The role and charter of the Medical Affairs Committee will remain intact. We are committed to continuing to listen to our providers and incorporating your thoughts into our policies that will ultimately serve the patients you treat every day. The combined health plan will also remain partially owned by the NC Medical Society, the NC Community Health Center Association, and Federally Qualified Health Centers.
Important Reminder: Billing Pre and Post 4/1/26
- For dates of service prior to 4/1/26, providers should submit WellCare Medicaid claims to Wellcare of North Carolina. Claims in this date range for WellCare members that are submitted to Carolina Complete Health will result in a rejection with notice: "Mbr not valid on DOS"
- For dates of service on or after 4/1/26, submit claims to Carolina Complete Health.
- If a member’s outpatient care overlaps these two date spans, please separate the claims by DOS and submit each to the appropriate entity.
- Physical health inpatient claims that span dates of service pre and post 4/1/26 should be billed to the health plan the member was enrolled with at the time of admission.
For claims with dates of service on or after 4/1/2026, providers should submit their claims to Carolina Complete Health using one of the following methods:
- Availity Essentials
- Carolina Complete Health Secure Provider Portal
- Clearinghouse/EDI: Payer ID 68069
- Mail: PO Box 8040 Farmington, MO 63640-8040
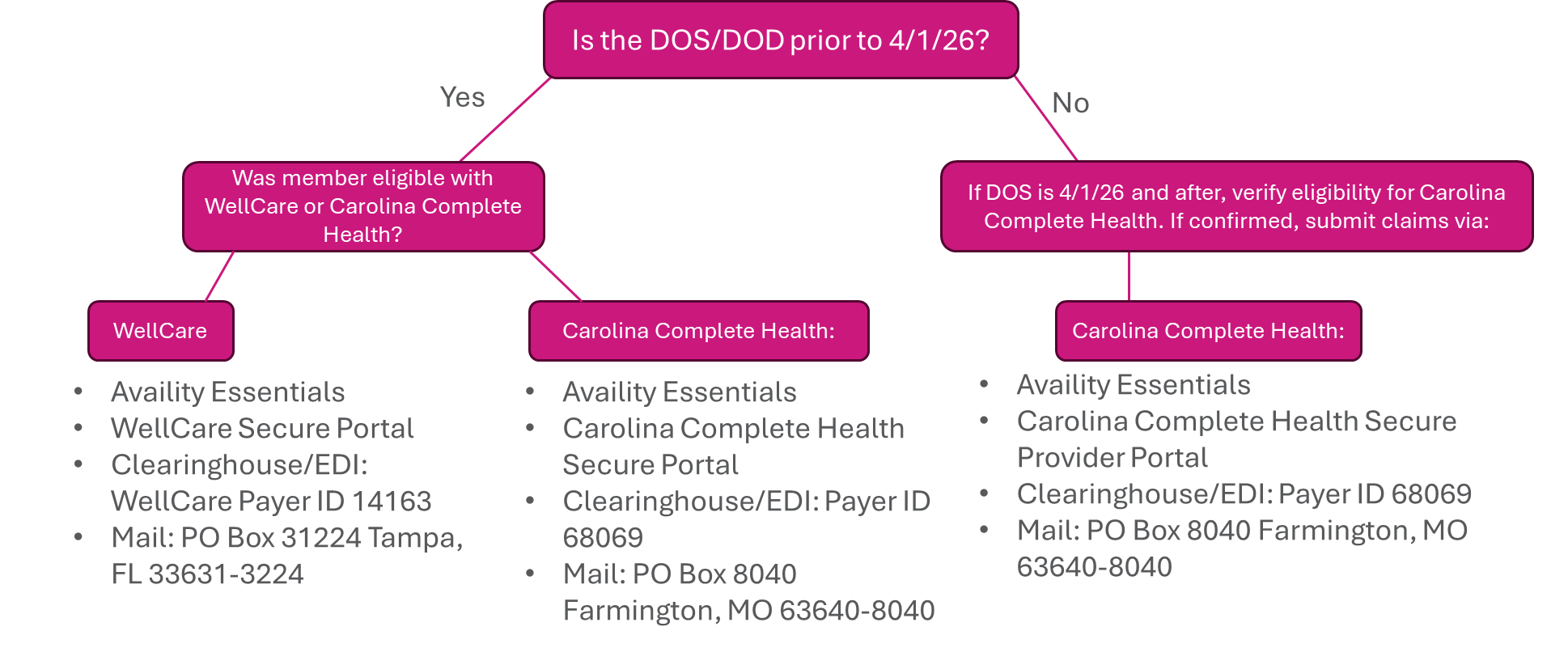
See below for more claims FAQs and review the claims decision tree:
Clinical Policy
Providers should continue to reference the policy pages on the Carolina Complete Health Network site, where current and upcoming policies are posted. Please refer to the following pages:
- Clinical Policies: All current policies approved by our Medical Affairs Committee.
- Policy Updates: Policies approved by our Medical Affairs Committee with future effective dates.
- Proposed Policy Revisions: Draft policies to be presented in the next Medical Affairs Committee meeting.
Provider Resources
- Quick Reference Guide (PDF)
- Provider Welcome Letter (PDF)
- Provider Manual (PDF)
- New Provider Orientation (PDF)
- General Compliance and Fraud, Waste and Abuse Training for Medical Providers Training (PDF)
For additional onboarding education, including Health Equity, view our Training page.
Provider Training
Merger Information Sessions
- February 19: Slides (PDF), Recording
- March 5: Specialty Focus: Behavioral Health, PT/OT/ST, DME Slides (PDF), Recording
- March 19: Slides (PDF)
- March 24: Specialty Focus: Home Health, PCS, EVV Slides (PDF), Recording
- April 2: Slides (PDF)
- April 16: Slides (PDF), Recording
Secure Provider Portal Training
Forms
Please use the forms below for dates of service April 1, 2026 and onward.
Panel Management:
For more, visit our Manuals, Forms, and Guides page.
Merger Frequently Asked Questions
Navigate directly to a topic:
Contracting and Network | Wellcare Medicare | Tailored Plans | Advanced Medical Homes and Clinically Integrated Networks | Claims and Billing | Payment and EFT | Panel Management | Website and Portals | Provider Relations | Outpatient Behavioral Health and ABA Services | Member Engagement, Benefits, VAS | Utilization Management | PT/OT/ST | Durable Medical Equipment | Care Management | Quality, Risk Adjustment | Home Health, PCS, EVV |

You will not need to sign a new agreement. Your existing WellCare agreement remains in effect after the merger and will cover members under the new state-wide unified health plan, named Carolina Complete Health.
You will not need to sign a new agreement. Your existing Carolina Complete Health agreement remains in effect after the merger and will cover members under the new state-wide unified health plan, named Carolina Complete Health.
One of your contracts was terminated so there would be only one agreement between you and the merged plan. Providers do not have to take action and will be considered in-network under the merged plan on
4/1/26.
Importantly, whichever contract is maintained for Medicaid will remain in effect after the merger and will cover members under the new state-wide unified health plan.
Contracts for Wellcare Medicare, Ambetter of North Carolina Inc., and Tailored Plan Physical Health with Trillium and Partners remain unaffected by the merger.
If you currently hold a Medicaid contract with Carolina Complete Health or WellCare of North Carolina, you will be considered in-network on 4/1/26, and therefore your members will stay assigned to you.
Additionally, with current WellCare Medicaid members being automatically transitioned to the unified health plan, these members will not need to change their PHP.
There is no re-credentialing or additional application process required as part of this merger on 4/1/26. Both health plans ingest provider infomation from NC Tracks. As long as the data is correct, there will be no need to notify when a new provider comes on board under the Tax ID. As long as the group NPI is already contracted, new individual NPIs are enrolled automatically.
Providers interested in contracting with the transportation vendor, MTM, may complete an application process through their website: https://www.mtm-inc.net/driverswanted/. You must be registered with NCTracks to proceed. Applications without this registration will be voided.
Wellcare Medicare will continue operating as it does today and will retain the Wellcare Medicare name. If you currently hold a Wellcare Medicare contract, it will remain active. Providers interested in joining the Wellcare Medicare network can submit a request through the online form.
There is no impact to members or to the provider contract for Medicare Wellcare. Those Medicare members will remain under the Wellcare banner and with the same ID as before.
When the two health plans integrate on 4/1/2026, the relationship between Carolina Complete Health and all four Tailored Plans will not change. Vaya and Alliance will continue to pay all of their own claims. Carolina Complete Health will continue to support Trillium and Partners by processing their physical health claims. Trillium and Partners will also continue to access Carolina Complete Health's physical health network for their membership. Please note that Trillium intends to begin processing physical health claims no sooner than July 1, 2026.
If provider is enrolled in NCTracks as an AMH3 and would like to continue in that role, we will ensure they are contracted accordingly. To confirm your contracting status, please email NetworkRelations@cch-network.com
As we approach the April 1, 2026 transition to the unified plan, please review the Patient Risk List (PRL) and Beneficiary Assignment File (BA file) distribution expectations below to ensure proper routing and processing.
Please note: The WellCare incoming folder is scheduled to remain operational through June 30 and will not be decommissioned prior to that date.
March 26, 2026 PRL (Pre-Merger)
- PRLs will be generated separately by Carolina Complete Health and WellCare of North Carolina.
- Providers/Clinically Integrated Networks (CINs) must return PRLs to the respective plan folder.
- PRLs returned to the incorrect plan folder may not ingest correctly and could cause delays.
April 26, 2026 PRL (Unified Plan)
- PRL will be generated by the Unified Plan (Carolina Complete Health).
- Returned PRLs (due May 7, 2026) should be submitted to the Unified Plan folders Carolina Complete Health
BA File Timeline
- Last weekly BA file (pre-merger): March 29, 2026
- Last monthly BA file (pre-merger): March 31, 2026
- First Unified Plan BA file: April 5, 2026
For questions, contact your Provider Engagement / Provider Relations representative or email providerengagement@cch-network.com.
Care management payments are issued by the 15th of each month. Provider can enroll for EFT for their care management capitated payments through Payspan by requesting the registration code for ALT payments.
For claims with a date of service prior to 4/1/2026, WellCare of NC and Carolina Complete Health will continue to process claims and encounters separately under timely filing guidelines.
For claims with a date of service on or after 4/1/2026, providers will submit their claims to the unified health plan. Claims will be processed in the Carolina Complete Health system.
For dates of service 4/1/26 and after, submit Standard Plan claims for the unified health plan using one of the following methods:
- Availity Essentials
- Carolina Complete Health Secure Provider Portal
- Clearinghouse/EDI: Payer ID 68069
- Mail: PO Box 8040 Farmington, MO 63640-8040
Legacy systems for WellCare of NC will remain operational for historical claim access. Historical claim access will be supported for 2 years post 4/1/2026. Two (2) years of historical claims will be accessible via the legacy provider portal.
For dates of service 4/1/26 and after, claims will be processed using the Carolina Complete Health claim systems and providers should use the Carolina Complete Health Payer ID (68069) if submitting through EDI/Clearinghouse.
The unified health plan will operate under the WellCare NC Tax ID Number and will be named Carolina Complete Health. If you are contracted with both entities and received a termination letter regarding one of your contracts, no action is required on your part. Your remaining contract will stay active, and you will continue to be considered in‑network as of April 1, 2026.
For dates of service 4/1/26 and after, standard plan Medicaid claims should be submitted to the unified health plan using one of the methods outlined below:
- Availity Essentials (selecting Carolina Complete Health as the payer)
- Carolina Complete Health Secure Provider Portal
- Clearinghouse/EDI: Carolina Complete HealthPayer ID 68069
- Mail: PO Box 8040 Farmington, MO 63640-8040
The Carolina Complete Health portal options include the Carolina Complete Health Secure Provider Portal and Availity Essentials. Providers who do not currently use the Carolina Complete Health portal may register after 3/1/26.
For dates of service on/after April 1, 2026, Medicaid claims should be submitted to unified health plan through the Carolina Complete Health Secure Provider Portal, Availity Essentials selecting Carolina Complete Health as the payer, EDI/Clearinghouse with Payer ID 68069, or via mail with paper claim forms.
Carolina Complete Health anticipates a seamless transition with no expected disruption to claims submission, processing, or payment timelines. Providers should continue to follow existing billing guidelines and established workflows, as no changes are required at this time. Systems and processes remain in place to support uninterrupted claims operations and timely payment.
Carolina Complete Health will pay the provider and then chase the primary insurance for Early and Periodic Screening, Diagnostic and Treatment services when there is Coordination of Benefits involved.
The process for claim corrections will follow the current Carolina Complete Health process.
- Contracted Providers: Submitters have 365 calendar days from the date of service to file a timely corrected claim.
- Non-Contracted Providers: submitters have 180 calendar days from the date of service to file a timely corrected claim.
Claim corrections can be completed through the Carolina Complete Health Secure Provider Portal, EDI, or through paper claim submission
Medical eye services with DOS on/after 4/1/26 that are performed by Doctors of Optometry (ODs) should be submitted to directly to Carolina Complete Health:
- Availity Essentials (selecting Carolina Complete Health as the payer)
- Carolina Complete Health Secure Provider Portal
- Clearinghouse/EDI: Payer ID 68069
- Mail: PO Box 8040 Farmington, MO 63640-8040
Routine vision services will continue to be billed to Centene Vision (formerly known as Envolve). For claim submission methods, review the Centene Vision Provider Manual.
For physical health inpatient or observation stays, claims should not be split billed. Whomever the member is effective with at the time of admission is responsible for the entire stay.
There will be no changes to obtaining DHB-2039s. Please submit the prior authorization to the health plan. Carolina Complete Health will fax the DHB-2039 along with the approved authorization. Nursing facilities will bill the health plan for services. For DOS on/after April 1, 2026, claims will be submitted to and processed by Carolina Complete Health:
- Availity Essentials (selecting Carolina Complete Health as the payer)
- Carolina Complete Health Secure Provider Portal
- Clearinghouse/EDI: Payer ID 68069
- Mail: PO Box 8040 Farmington, MO 63640-8040
After 90 consecutive days in a nursing facility, the member is disenrolled from NC Medicaid Managed Care to NC Medicaid Direct on the first day of the month following the 90th consecutive day in the nursing facility.
Claims submitted to WellCare for services rendered on or after 4/1 will be rejected as “Member Not Eligible on The Date Of Service”. Providers will be expected to follow their normal process of identifying the correct health plan for that member.
For HHAx related claims, providers should expect to receive a rejection advising “Patient Not Found or Visits Cannot Be Imported Prior to Patient SOC Date or After Patient Discharge Date" if a claim is submitted with the wrong Payer ID.
For WellCare claims, recoupment letters will continue to be issued and managed through WellCare’s existing recovery processes while run‑out claims remain active. During this period, any negative balances will continue to be tracked and managed consistent with current WellCare and Carolina Complete Health practices.
Carolina Complete Health offers a free solution for payment by Electronic Funds Transfer (EFT) and Electronic Remittance Advice (835)/Explanation of Payment (ERA/EOP) through PaySpan®. If you are not already registered, create a new account by registering at payspanhealth.com or calling 1-877-331-7154, option 1.
Claims with dates of service 4/1/26 or after will be processed by Carolina Complete Health and the remittance will be designated as Carolina Complete Health. Providers can receive electronic funds transfer and electronic remittance through PaySpan. To register for Payspan, view the Payspan Provider Guide.
Remits will be available through the Carolina Complete Health Secure Portal, Payspan, and Availity.
The health plan will use the North Carolina Medicaid fee schedule as a basis for provider reimbursement. Please refer to your specific provider agreement and for questions, contact Provider Relations to assess and provide any necessary clarification.
Carolina Complete Health's check run schedule occurs weekly on Monday, Wednesdays, and Fridays. Payment is issued to providers the following business day. Providers can continue using Payspan, a free solution that provides electronic payment and remittance. If providers already use Payspan for WellCare, but not Carolina Complete Health, you can add a line-of-business with a new registration code (provided by Payspan) to set up EFT/ERA with Carolina Complete Health. Contact Payspan via email or phone: PayspanProviderSupport@zelis.com or 1-877-331-7154. This will also be discussed live in the Claims Section. Thank you.
We are closely monitoring our market share, and while we are close to the cap in a couple of regions, we do not believe the cap will have a material impact on our membership. We are also actively working with the State to ensure compliance. The State will make auto-assignment adjustments to address a situation where we are over the cap. This will take place beginning 4/1/2026.
The necessary adjustments to stay under the cap would be handled through the State’s auto-assignment process, and we do not anticipate manual reassignments. For regions where the combined member enrollment reaches the 40% ceiling, the Department will turn-off auto-assignment to Carolina Complete Health until the member enrollment falls below 40%. This will take place beginning 4/1/2026.
Carolina Complete Health will adopt the current WellCare process for providers requesting member reassignment. Carolina Complete updated the member reassignment request worksheet to an excel sheet that can be securely emailed to the Provider Engagement team to process bulk member moves. This form can be found online https://network.carolinacompletehealth.com/forms under Panel Management Forms.
For dates of service occurring on or after April 1, 2026, providers may use the Carolina Complete Health Secure Provider Portal or Availity Essentials (selecting Carolina Complete Health as the payer).
Please note that Ambetter of North Carolina Inc., Trillium Health Resources, and Partners Health Management will continue operating on their respective portals. No changes to these lines of business.
Providers are able to:
- Check eligibility
- Submit, correct, and check claim status, including batch claims
- View Payment history
- Submit and check status of Prior Authorizations
- Access Health Records & Assessments
- View AMH Reports
- View Care Gaps
- Quality and Risk Adjustment Reports if applicable
Feel free to reach out to the Provider Engagement team via email for portal support at ProviderEngagement@cch-network.com.
The unified health plan will use the existing Carolina Complete Health secure portal, for dates of service 4/1/26 and after. Providers who have never used this portal (those who currently hold WellCare Medicaid contracts only and will be new to the Carolina Complete Health network) may register for this portal beginning 3/1/26. Our provider education and engagement teams will host portal trainings beginning 2/26/26. Providers may also use Availity Essentials to submit claims and authorizations electronically.
For Carolina Complete Health providers, the public Carolina Complete Health Network website will remain. WellCare providers should begin using this webpage upon go-live for updated materials (i.e. provider and billing manuals, contacts, and provider tools).
Legacy systems for WellCare of NC will remain operational for historical claim access. Historical claim access will be supported for 2 years post 4/1/2026. Two (2) years of historical claims will be accessible via the legacy provider portal.
For dates of service 4/1/26 and after, providers should use the single unified health plan portal (Carolina Complete Health Secure Portal) or Availity Essentials (selecting Carolina Complete Healthas the payer) to check eligibility, submit claims, authorizations, and more.
Yes, a Portal Acct Mgr (PAM) can give Manage User access to other portal users under the same TIN.
Provider Relations
The structure of the Provider Experience team is a blend of WellCare and Carolina Complete Health team members. For provider assignments, please visit the Provider Engagement Team page. For historical claim inquiries with WellCare for dates of service prior to April 1, please continue submitting to ncproviderrelations@wellcare.com
When calling the WellCare Provider Services Call Center, providers will be informed of the merger and directed to the call center of the unified health plan, under the Carolina Complete Health name. In the message they will be provided with the 1-833-552-3876 number for future calls and informed that post 6/30/26 the WellCare line will no longer be in service.
Yes. There will be bi-weekly information sessions beginning 2/19/26. Secure provider portal trainings will launch on 2/26 and will occur bi-weekly. We will also share regular updates through provider bulletins and newsletters. Providers should also bookmark the integration landing page where new resources and training will be posted. You may also reach out to your Provider Engagement representative at anytime with questions.
The structure of the Provider Experience team is a blend of WellCare and Carolina Complete Health team members. For provider assignments, please visit the Provider Engagement Team page. For historical claim inquiries with WellCare for dates of service prior to April 1, please continue submitting to ncproviderrelations@wellcare.com
Yes, behavioral health outpatient services will require prior authorization, similar to the current requirements. Individual, group and family therapy requires authorization for units beyond the first 24 per fiscal year (resets on July 1 each year). The following codes apply for outpatient therapy authorizations: 90832, 90834, 90837, 90846, 90847, 90849, and 90853. Authorization requirements remain unchanged for other outpatient services, including Research Based Behavioral Health Treatment for Autism Spectrum Disorder (i.e. ABA), as well as peer support services beyond unmanaged units, and psychological/neuropsychological testing beyond unmanaged units. Providers should also refer to the Carolina Complete Health Pre-Auth Tool for the most up to date authorization requirements.
*This is specific to outpatient psychotherapy: 90832, 90834, 90837, 90846, 90847, 90849, and 90853*
Carolina Complete Health and WellCare of NC allow 24 unmanaged visits for BH outpatient psychotherapy for any combination of the following codes: 90832, 90834, 90837, 90846, 90847, 90849, and 90853
- Units will NOT reset to zero on 04/01/2026
- Carolina Complete Health’s 24 count began on 02/01/26 and will reset on July 1, 2026
- For former WellCare of NC members, if there is NOT an active auth on file, then the system would start counting the 24 limits as though the members had always been CCH members (from 2/1/26).
- IF an authorization is already on file with WellCare for BH outpatient therapy, this authorization will transition to Carolina Complete Health. The provider should follow the authorization already on file.
All visits will reset on July 1, 2026 and every July 1 thereafter.
*Even when using unmanaged visits, ALL services delivered must be medically necessary and all documentation requirements should still be present in members’ records.
The structure of the Provider Experience team is a blend of WellCare and Carolina Complete Health team members. For provider assignments, please visit the Provider Engagement Team page. For historical claim inquiries with WellCare for dates of service prior to April 1, please continue submitting to ncproviderrelations@wellcare.com
Active open authorizations will transfer over to the unified health plan. Authorization requirements remain unchanged for Research Based Behavioral Health Treatment for Autism Spectrum Disorder. Providers should refer to the Carolina Complete Health Pre-Auth Tool for the most up to date authorization requirements.
WellCare Medicaid members received an announcement letter in January, followed by a series of informational materials delivered through multiple channels and platforms. These may include, but are not limited to, direct mail, text message onboarding journeys, paid media (digital and traditional), social media (paid and organic), public relations, and grassroots activities across all six regions.
These communications will ensure that members understand what is changing, what is staying the same, and how to access their benefits. No action will be required from members, and there will be no impact on their current Medicaid coverage.
Medicaid members will keep the same Medicaid ID number and it will be printed on the Member ID card. WellCare Medicaid members will be sent a new Carolina Complete Health ID card and welcome packet before 4/1/26
Members are assigned at the Advanced Medical Home (AMH) group level and this will be listed on the member ID card.
Current recipients will stay enrolled and will automatically transition to the unified health plan, named Carolina Complete Health effective 4/1/26. WellCare of North Carolina will no longer be listed with the Enrollment Broker beginning February 15, 2026.
WellCare of North Carolina will no longer be listed with the Enrollment Broker beginning February 15, 2026.
Members can access many Value-Added Services by simply filling out a webform available through our website at www.carolinacompletehealth.com/vas. Some Value-Added Services require that the member connect with care management or call a specific number. Information on all Value-Added Services is available on the website or by calling Member Services at 1-833-552-3876 (TTY: 711).
Children under 21 years of age are covered by Medicaid for this benefit, Carolina Complete Health will continue covering it as a Value-Added Services for adults 21+.
- Enhanced Hearing Benefit for Members Age 21+
- Covers the cost of a hearing aid, for members 21 and older, if medically necessary.
- Limited to every 2 years HCPCS Codes V5014, V5050, V5060, V5090, V5110, V5130, V5160, V5240, V5241, V5264, V5266, V5267, V5274, V5299.
Providers can verify member eligibility electronically with the Carolina Complete Health secure provider portal or Availity Essentials. Providers can also verify by calling Member Services 1-833-552-3876.
For dates of services 4/1/26 and onward submit authorizations to Carolina Complete Health unless the service falls to one of the UM Vendors, outlined below.
| Service Scope | Current Carolina Complete Health vendor | Current WellCare of North Carolina vendor | Carolina Complete Health Merged Plan 4/1/26 and onward |
|---|---|---|---|
| Radiation Oncology | None | Evolent | Evolent: effective no earlier than 5/1/26 |
| Musculoskeletal Surgery | None | Evolent | Evolent: effective 4/1/26 |
| Interventional Pain Management | None | Evolent | Evolent: effective 4/1/26 |
| Advanced Imaging | Evolent | Evolent | Evolent |
| Physical, Occupational, Speech Therapy | None | Evolent | None. Submit directly to health plan. |
| Cardiovascular Procedures | None | Evolent | TurningPoint: effective 5/1/26 |
| Sleep Diagnostics | None | EviCore | None. Submit directly to health plan. |
| Genetic Testing | None | EviCore | EviCore effective 5/1/26. |
Active open authorizations will transfer over to the unified health plan. Historical authorizations (past 18 months prior to 4/1/26) will also migrate over. If a service was approved before 4/1/26 but is performed on or after 4/1/26, the claim will pay correctly when filed with Carolina Complete Health. For example, an authorization is requested and approved for a 60-day period from 3/15/26 - 6/15/26. The authorization will be valid for services provided after 4/1/26, even though it was approved while the member was covered under WellCare of NC prior to the integration date. Providers can view authorizations in the secure provider portal.
There will not be a waiver period for current WellCare Medicaid members. For services provided to WellCare of NC members before April 1, 2026, continue submitting authorization requests through WellCare or the appropriate WellCare vendor using the WellCare NCProvider Portal, the vendor portal, fax, or phone.
Active open authorizations will transfer over to the unified health plan. Historical authorizations (past 18 months prior to 4/1/26) will also migrate over. If a service was approved before 4/1/26 but is performed on or after 4/1/26, the claim will pay correctly when filed with Carolina Complete Health. For example, an authorization is requested and approved for a 60-day period from 3/15/26 - 6/15/26. The authorization will be valid for services provided after 4/1/26, even though it was approved while the member was covered under WellCare of NC prior to the integration date. Providers can view authorizations in the secure provider portal.
The topic of Utilization Management will be covered in our Provider Information Sessions launching 2/19/26. Additionally, there will be necessary updates made to our Provider Manual plus additional resources, such as a UM Quick Reference Guide, developed for provider guidance. Beginning April 1, 2026, providers may call Provider Services at 1-833-552-3876 to reach medical management and care management departments. Provider may also work directly with their designated Provider Engagement and Relations representative.
Providers should always use the Prior Authorization Lookup Tool to confirm whether a prior authorization is required before rendering services.
For chiropractic services, prior authorization is required only for non-participating providers for the following CPT codes: 98940, 98941, 98942, & 98943. Participating providers do not require prior authorization for these codes. Authorizations for services on/after April 1 may be submitted via the Carolina Complete Health Secure Provider Portal, Availity Essentials, by phone or via fax.
eviCore will be utilized to review genetic testing for the merged Carolina Complete Health plan, and the authorization requirements will be similar to what WellCare of NC has in place currently.
Also utilize the Carolina Complete Health Pre-Auth Check Tool for details
Providers may request a retrospective review up to 90 days after the date of service (DOS) or the date of admission (DOA) in the case of an inpatient request. Please submit a request for retrospective authorization in the same manner that you submit a preauthorization. For guidance reference our Provider Guide (PDF). Please note that a retrospective review is an initial review of services provided to a beneficiary, but for which authorization and/or timely notification to Carolina Complete Health was not obtained due to extenuating circumstances. Examples of extenuating circumstances include, but are not limited to the following:
- The member was unable or refused to provide eligibility information (i.e., member unconscious).
- Services were authorized by another payer, who subsequently determined the member was not eligible at the time of service or that the services occurred during a transition of care period.
- A catastrophic event/natural disaster interfered with normal business operations.
- A service/procedure change due to unavoidable circumstance.
No. Authorization is not required when Carolina Complete Health is acting as the secondary payer.
Authorization is required if:
• Primary benefits have terminated
• Primary payer benefit maximums are reached or nearly reached
• The primary payer issues a denial
Skilled Nursing Facilities
To streamline processes for nursing facility admissions and the determination of long-term care financial eligibility, NC Medicaid created a new standardized PHP Notification of Nursing Facility Level of Care Form (NC Medicaid-2039) for PHPs and nursing facilities to communicate with local Departments of Social Services (DSS).
The standardized form includes all information a local DSS needs to begin the financial determination for long-term care as required by the Centers for Medicare and Medicaid Services (CMS). Once counties conduct the financial determination and establish the patient monthly liability (PML), the PML will be shared with health plans and allow payments to proceed to nursing facilities.
To further clarify how this process works, NC Medicaid created stakeholder-specific fact sheets for counties, for health plans, and for providers (including hospitals and nursing facilities). The fact sheets outline the information flow, timelines and requirements for the long-term care financial eligibility determination process.
• County Fact Sheet
• Provider Fact Sheet
Effective 4/1/26, PT/OT/ST authorizations can be submitted directly to the unified health plan. Providers should submit authorization requests to the health plan through the Carolina Complete Health Secure Portal, Availity Essentials, phone or fax. Please use the Pre-Auth Tool to check on a specific service or procedure.
Required documentation includes:
- Signed MD Order within the last 6 months
- Evaluation/progress notes from the past 3 months Plan of Care
- For continuations: new order (if previous is signed & dated longer than 6 months ago) and an updated plan of care stating frequency and duration of therapy.
The health plan sets up authorizations using umbrella codes for each discipline. PT is 97110, OT is 97530 and ST is 92507. Providers can submit their requests with these umbrella codes for even faster processing. Other covered therapy codes can be billed for each discipline based on services provided at each visit, but we designate the prior authorization per these umbrella codes to ensure that each therapy discipline can be accessed for the dates of service needed.
The discharging clinic can call or fax to request that a prior authorization is ended early due to therapy services ending at their facility via CCH phone number 1-833-552-3876 or fax: 833.238.7694. Please be prepared to include the member name, date of birth, authorization number, therapy provider, specific therapy discipline and date of discharge.
For services April 1 and onward, PT/OT/ST authorizations should be submitted directly to the health plan, Carolina Complete Health: How to Secure a Prior Authorization
How do providers request an extension for unused speech therapy visits on an existing authorization?
- Providers may request an extension by calling Provider Services at 1-833-552-3876.
- Requests must be submitted prior to the authorization end date and should include the requested new end date for the authorization.
Yes. Blood pressure monitors and cuffs are part of Durable Medical Equipment benefits that NC Mediaid provides.
For Physical Rehabilitation Equipment and Supplies, providers must follow the North Carolina Medicaid Clinical Coverage Policy 5A-1.
Key requirements include:
- A valid provider order
- Documentation supporting medical necessity
- Adherence to coverage guidelines outlined in the policy, which provide clear direction for most types of durable medical equipment (DME)
Benefit counts will carry over from WellCare and these will not reset effective 04/01/26. Providers should continue to follow policy limits as outlined in policy.
To notify Carolina Complete Health of pregnancy, please complete the Pregnancy Risk Screening Tool from NC DHHS and fax to Carolina Complete Health Care Management Notification of Pregnancy (NOP): 833-238-7689. NOPs can also be completed using the Carolina Complete Health Secure Provider Portal within the assessments tab in the member's health record. Early notification of pregnancy allows the health plan to assist the beneficiary with prenatal care coordination of services.
A global authorization number is not provided by Carolina Complete Health upon submission of a NOP. Instead, the hospital shall notify Carolina Complete Health of admission within one business day. Upon admission and notification, an inpatient authorization will be generated.
Quality performance data remain accessible via Carolina Complete Health secure provider portal and report packets sent prior to Quality meeting. Carolina Complete Health’s current incentive model will continue for the merged entity. Measures, targets for each year will be distributed through assigned Provider Engagement teams. Providers will continue to use Carolina Complete Health’s Provider Portal.
CoC agendas for Medicaid will look like the current Carolina Complete Health agendas.
The Quality Incentive program will be unified, aligning with NC DHB guidelines and current Carolina Complete Health model. All reporting for the program will be combined effective 4/1.
For the merger, both Carolina Complete Health and WellCare Medicaid members will be combined on the same platform. The CoC program will be deployed with Carolina Complete Health Medicaid members initially and subsequent waves of agendas will include current WellCare members. Medicare agendas will remain on the system currently used in previous years with Wellcare Medicare. Providers can continue accessing CoC agendas through the Carolina Complete Health secure provider portal. Providers will also have the same paper and fax options available for submission.
Supplemental data and documentation loaded into the WCNC portal will transition to the Carolina Complete Health portal and current Carolina Complete Health process for supplemental data uploads will continue post transition.
For PCS a new provider cannot begin services or obtain authorization if the previous provider has not been properly discharged.
To change PCS providers, the following process must be completed:
- The 3051 form must be submitted, completing:
- Member demographic information (top section)
- Section F (Change of Provider)
- The form should be faxed to 1-833-706-0238
Providers should make every effort to ensure a discharge is in place with the current provider before initiating this request.
In some cases, the member or their family (for minors) may need to request discharge from the current provider to allow services to begin with a new provider.
Please note:
- Overlapping dates of service are not permitted for PCS
- Authorization for a new provider cannot be approved until the transition is completed
Expedited requests may be considered in certain situations, including:
- PCS agency closure
- Member has already been discharged by the current provider
- Member is moving between Adult Care Homes (ACH)
The codes for PCS will not change. The Home Health codes subject to EVV, for Carolina Complete Health, can be found here.
Carolina Complete Health will send a new placement and authorization. This will create a new member record and the WellCare member record will be discharged. Please do not manually create a member/auth and do no add additional contracts to the existing WellCare record. Manual changes from the provider portal will result in billing issues.
If you are a new agency for PCS, we will allow members the opportunity to select the agency of their choice. If the member has no preference we will direct them to our “find a provider tool” to select an agency of their choice. Often, as we are looking to meet the members’ needs, we will do outreach to agencies to see who has capacity to service the needs of members in each region and share these across the Care Management team.
Yes, submit DHB-3051 to Carolina Complete Health with the “Change of Provider” section completed. The new providers are responsible for notifying Carolina Complete Health of any discharges. The new PCS provider has 7 days to submit a service plan to Carolina Complete Health.
No. Diagnosis codes will not automatically populate on authorizations sent to HHAeXchange. Providers are responsible for entering the appropriate primary diagnosis code when working with authorizations.
To ensure accurate billing and avoid claim rework, providers should reference clinical documentation (such as RN assessments or care plans) to identify the correct diagnosis code associated with the member’s condition.
Do you have a Carolina Complete Health member who is in need of initial PCS?
- The CCH Personal Care Services Request "3051" Form is to be completed by member's primary care provider or attending physician. This can be found on the Manuals, Forms, and Guides page.
- Fax the 3051 form to Carolina Complete Health Care Management: 1-833-706-0238
- Once this form is received a face to face visit will be scheduled within 30 days by CCH Care Manager
- After assessment is completed and start of care date is determined, an authorization will be created by CCH and will be shared with the agency. This document will include purchased tasks to be completed by PCS attendant. Agencies will receive the authorization via fax and can also view on the CCH Secure Provider Portal.
Reauthorization of Personal Care Services
- Providers do not need to request reauthorization of PCS.
- CCH LTSS Care Managers are responsible for reauthorizing personal care services through comprehensive face-to-face visits and assessments.
- Providers can access member health records, assessments and authorization status through the Secure Provider Portal. For support in navigating the Secure Provider Portal, reach out to your Provider Engagement Administrator.
Questions?
- Please contact our customer service department at 1-833-552-3876. If the member is in active care management for PCS, you may request to speak to the assigned Care Manager or LTSS Manager.
Face to face assessments are not required, however, there needs to be a written order or verbal order documented.
For Home Health Care Services, if EVV data is not submitted, the claim will not immediately reject. When the claim is billed directly to Carolina Complete Health without EVV data, it is placed on a 14-day hold to allow time for the EVV visit to be submitted via HHAeXchange and matched with claims data received. If an EVV match is not found within the 14-day hold period, the claim will then be denied "EXev" unless otherwise denied immediately for a reason unrelated to EVV.
Please note: Claims for personal care services must be submitted through HHAeXchange and will deny "EXev" if a provider attempts to bill directly to the health plan.
Claims submitted to WellCare for services rendered on or after 4/1 will be rejected as “Member Not Eligible on The Date Of Service”. Providers will be expected to follow their normal process of identifying the correct health plan for that member.
For HHAx related claims, providers should expect to receive a rejection advising “Patient Not Found or Visits Cannot Be Imported Prior to Patient SOC Date or After Patient Discharge Date" if a claim is submitted with the wrong Payer ID.
HHAeXchange will link existing WellCare of NC connected agencies to the Carolina Complete Health Secure Provider Portal as part of the transition. A system review has been completed to identify providers who are new to Carolina Complete Health and most links will be established automatically before go-live.
Providers will continue to have the ability to add and manage billing diagnosis codes within the HHAeXchange system. Detailed requirements and additional guidance are available in the HHAeXchange Knowledge Base:
Carolina Complete Health builds authorizations for Personal Care Services for a six month authorization span. Within the authorization span, each calendar month will be broken out as its own line item. For example, Line 1: 2/1/26-2/28/26, Line 2: 3/1/26-3/31/26, Line 3: 4/1/26-4/30/26, Line 4: 5/1/26-5/31/26, Line 5: 6/1/26-6/30/26, Line 6: 7/1/26-7/31/26.
The date of service will determine the appropriate payer for submitting visit data and billing through Electronic Visit Verification. If the date of service is prior to 4/1/26 and the member was covered by WellCare of North Carolina, the visit and claim will need to be confirmed and billed against the WellCare NC Contract. If using HHAeXchange, select the member record associated with WellCare. When a claim is submitted after 3/31/26 for services provided before 4/1, members previously covered by WellCare of North Carolina will show a “discharged” status in the HHAX portal under the WellCare NC record.
All visits with dates of service 4/1/26 and after will be confirmed/billed against the CCH member record.
Use the following Payer IDs if using a third party EVV vendor:
Dates of Service Prior to 4/1/26 for WellCare Medicaid members:
- WellCare PCS Payer ID: 23937
- WellCare HHCS Payer ID: 57538
Dates of Service 4/1/26 and after:
- Carolina Complete Health PCS Payer ID: 24075
- Carolina Complete Health HHCS Payer ID: 57535
- Use payer ID 68069 for HHCS claims that are billed directly to the health plan when the date of service is 4/1/26 or later.
