Tailored Plans
What are Tailored Plans?
A Tailored Plan is an integrated health plan for individuals with significant behavioral health needs or intellectual/developmental disabilities. Tailored Plans are required to contract with a licensed prepaid health plan, such as Carolina Complete Health.
Beginning April 1, 2026, Carolina Complete Health will be serving all four Tailored Plains: Alliance Health, Partners Health Management, Trillium Health Resources, and Vaya Health.
- Alliance and Vaya will continue managing their own provider networks. Carolina Complete Health will continue contracting for physical health providers for Trillium and Partners.
- For Alliance and Vaya, Carolina Complete Health will provide Nurse Advice Line services.
- For Trillium and Partners, Carolina Complete Health will continue to process physical health claims*, provide utilization management functions, serve in a secondary care management role for some members, provide Nurse Advice Line services, and some of the other same services and supports that have historically been provided. *Trillium intends to pay its own physical health claims as early as 7/1/2026.
Beneficiaries who qualify for a Tailored Plan are auto enrolled into a Tailored Plan based on their region. This model for the Tailored Plans went live on July 1, 2024, and until that point, they are considered Local Management Entities (LMEs). Tailored Care Management went live on December 1, 2022.
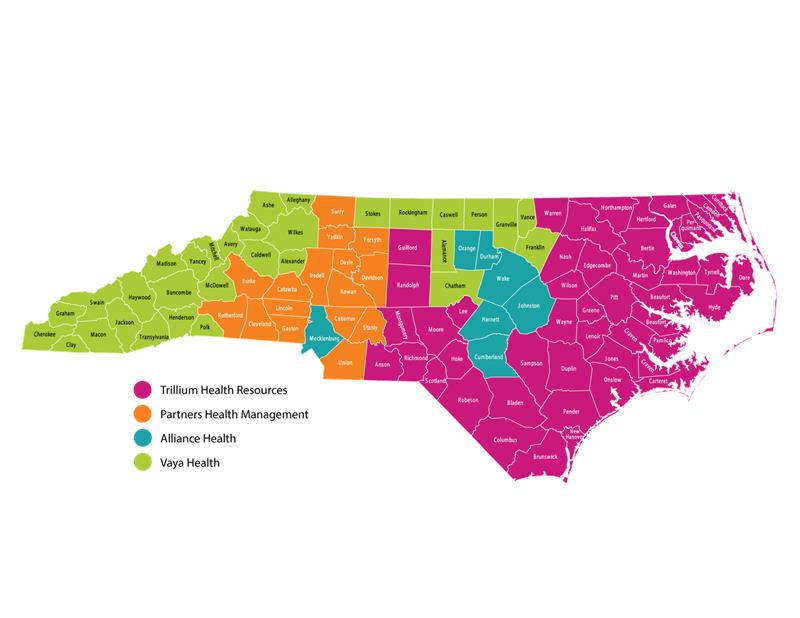
- Alliance Counties: Cumberland, Durham, Harnett, Johnston, Mecklenburg, Orange, and Wake
- Partners Counties: Burke, Cabarrus, Catawba, Cleveland, Davidson, Davie, Forsyth, Gaston, Iredell, Lincoln, Rutherford, Stanly, Surry, Union and Yadkin.
- Trillium Counties: Anson, Beaufort, Bertie, Bladen, Brunswick, Camden, Carteret, Chowan, Columbus, Craven, Currituck, Dare, Duplin, Edgecombe, Gates, Greene, Guilford, Halifax, Hertford, Hoke, Hyde, Jones, Lee, Lenoir, Martin, Montgomery, Moore, Nash, New Hanover, Northampton, Onslow, Pamlico, Pasquotank, Pender, Perquimans, Pitt, Randolph, Richmond, Robeson, Sampson, Scotland, Tyrrell, Warren, Washington, Wayne, Wilson.
- Vaya Counties: Alamance, Alexander, Alleghany, Ashe, Avery, Buncombe, Caldwell, Caswell, Chatham, Cherokee, Clay, Franklin, Graham, Granville, Haywood, Henderson, Jackson, Macon, Madison, McDowell, Mitchell, Person, Polk, Rowan, Rockingham, Stokes, Swain, Transylvania, Vance, Watauga, Wilkes, and Yancey
Contracting
Providers are encouraged to contract with each Tailored Plan in their service area, but it is not required. However, PCPs who contract with fewer Tailored Plans risk losing beneficiaries.
Partners and Trillium leverage the Carolina Complete Health physical health provider network. A physical health provider wishing to participate in the Partners or Trillium Tailored Plan network should complete the contract request form with Carolina Complete Health.
Alliance and Vaya and Alliance have their own provider networks. A provider wishing to contract with Vaya or Alliance should contact the Tailored Plan.
- Alliance Provider Support: 855-759-9700
- Vaya Provider Support: 1-828-225-2785 ext. 1512
Partners and Trillium Physical Health Provider Resources
Frequently Asked Questions
Whether you receive your payments via paper check or ACH you will find them on the Payspan portal, via Payspanhealth.com. For providers not yet enrolled, visit the Payspan Portal and click register or contact Payspan: Call 1-877-331-7154, Option 1 – Monday thru Friday 8:00am to 8:00pm EST. Also see attached guide. Using Payspan to Access Medical Home Payments (PDF)
Reach out to your CCHN Provider Engagement Administrator if you have any difficulty or questions, they are assigned by county.
If you do not have a contract for the Tailored Plan network, you will be considered ‘out-of-network’ and could be subject to reduced reimbursement rates for physical health services.
Our team of network professionals is available to assist you in meeting critical dates for contracting. Please utilize our Contract Request Form.
To be considered 'in-network’ and eligible for the full reimbursement rate for physical health services for Standard Plan members, providers should also be contracted with CCH for Standard Plan. Please see our Join the Network page for more information.
